Photo: Tel Aviv University
Researchers at Tel Aviv University revealed a stunning breakthrough when they published a study demonstrating how they were able to 3D print the world's first vascularized engineered heart. Using a patient's own cells and biological materials, the 3D-printed heart is an incredible success story that could change the way we think about regenerative medicine.
Until now, scientists have only been able to print simple tissue samples. But with the successful printing of a functioning heart filled with blood vessels, chambers, cells, and more, the field has taken a big step forward. The study will also give hope to the thousands of men and women waiting for heart transplants, as there is a shortage of donors.
“This heart is made from human cells and patient-specific biological materials. In our process these materials serve as the bioinks, substances made of sugars and proteins that can be used for 3D printing of complex tissue models,” says Professor Tal Dvir of Tel Aviv University's School of Molecular Cell Biology and Biotechnology and Sagol Center for Regenerative Biotechnology, who led the research for the study. “People have managed to 3D-print the structure of a heart in the past, but not with cells or with blood vessels. Our results demonstrate the potential of our approach for engineering personalized tissue and organ replacement in the future.”
The initial 3D-printed organ is about the size of a rabbit's heart, but the plan is to scale up. The study, which was conducted jointly by Prof. Dvir, Dr. Assaf Shapira of TAU's Faculty of Life Sciences, and Nadav Moor (a doctoral student in Prof. Dvir's lab), first required them to perform a biopsy on fatty tissue from patients. The cellular and a-cellular materials were then separated, with the cells reprogrammed to become pluripotent stem cells. Other materials like collagen were used as “ink” during the printing.
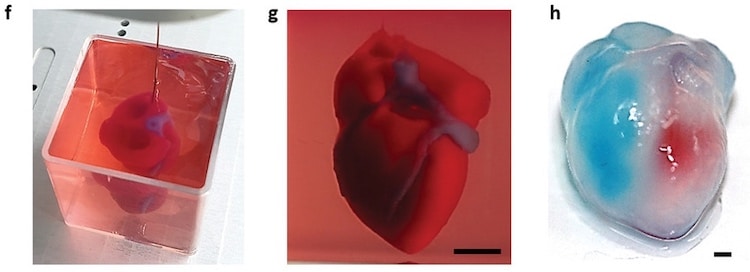
f,g) A printed heart within a support bath. h) After extraction, the left and right ventricles were injected with red and blue dyes, respectively, in order to demonstrate hollow chambers and the septum in‐between them. (Photo: Dvir, Shapira, Noor, et al.)
By using biomaterials from patients, the researchers eliminate the risk of implant rejection. This devastating occurrence is a reality for most patients receiving organ transplants, with approximately 50% of organ donations being rejected by the body within 10 to 12 years. This breakthrough is a big step forward in bringing down that percentage.
“Ideally, the biomaterial should possess the same biochemical, mechanical and topographical properties of the patient's own tissues,” explains Prof. Dvir. “Here, we can report a simple approach to 3D-printed thick, vascularized and perfusable cardiac tissues that completely match the immunological, cellular, biochemical, and anatomical properties of the patient.”
The next step is culturing the 3D-printed hearts, teaching them how to behave, and then transplanting them into animal models. Prof. Dvir notes that at the moment the cells can contract, but they need to learn how to pump so that they can work together. While there's a lot of work ahead, he is optimistic about the technology. “Maybe, in ten years, there will be organ printers in the finest hospitals around the world, and these procedures will be conducted routinely.”
Watch as Israeli scientists create the world's first 3D-printed heart.
Related Articles:
Revolutionary Technology Helps Spinal Injury Patients Take Their First Steps
Scientists Say Tribe in Bolivian Rainforest Have the “Healthiest Hearts in the World”
Contact Lenses That Darken in Sunlight for UV Protection Could Go on Sale Soon
Groundbreaking Brain Surgery Allows Quadriplegic Patient to Move His Hand Again