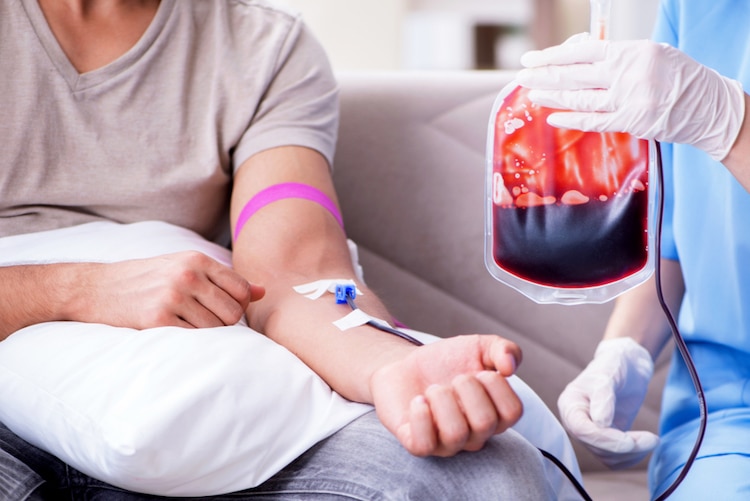
Stock Photos from Elnur/Shutterstock
According to the Red Cross, someone needs a blood transfusion every two seconds in the United States, which is why health organizations are constantly reminding us that donating blood is important. Continuous donations are necessary not only to keep a good worldwide supply—blood can only be used for a limited time after donation—but also to ensure that all blood types are readily available. Now, in a stunning breakthrough, scientists from the University of British Columbia have found a way to convert blood into a type that can be accepted by almost any patient.
As most of us know, humans have blood types broken down into four major groups—A, B, AB, and O. People with type O are considered universal donors, as their blood is compatible with anyone having A+, B+, AB+, or O+ blood. To put it into perspective, 75% of the population has Rh-positive blood. Having more type O blood readily available means less worry when transfusions are necessary. Researchers were able to convert type A blood into type O blood using gut bacteria, a discovery that could have an impact on millions of patients who require blood transfusions.
Though the transformation only occurred in a petri dish and more research will be necessary to make it a viable method for patients, the medical community is already excited by the possibilities. Postdoctoral researcher Peter Rahfeld and a team of colleagues are responsible for finding a way to break down the antigens that cause blood incompatibility using a bacterial enzyme from the human gut.
To make it more clear, blood groups are determined by the presence of two antigens (A and B) on the surface of red blood cells. If you have type A blood, you have A antigens on your red blood cells and therefore can only receive blood from a source that also has A antigens (type A) or neutral antigens (type O). Obviously, this is quite limiting, as it cuts out 50% of the blood type possibilities. If you are type O, you can donate to everyone, but you can only receive from type O, as all the other blood types contain antigens that will be rejected by the body.
In their experiment, antigens in type A blood were transformed from A antigens into H antigens—a neutral antigen found in type O blood. After cultivating a bacteria called Flavonifractor plautii from human stools, the team isolated two enzymes that can remove components of the A antigen, effectively converting them into the neutral H antigen. When added to type A blood, the enzymes transformed the antigens, creating type O blood that could be accepted by anyone who is Rh positive.
“Their ability to completely convert A to O of the same rhesus type at very low enzyme concentrations in whole blood will simplify their incorporation into blood transfusion practice, broadening blood supply,” write the researchers.
The scientists will now continue their research to ensure that the enzymes completely wipe out all traces of the A antigen. If successful, they could effectively double the blood supply by making type A blood available to anyone who needs a transfusion.
h/t: [News Medical]
Related Articles:
World’s First 3D-Printed Heart Could Revolutionize Organ Transplants
Revolutionary Technology Helps Spinal Injury Patients Take Their First Steps
Groundbreaking Brain Surgery Allows Quadriplegic Patient to Move His Hand Again
2018 Nobel Prize in Medicine Goes to Researchers Who Revolutionized Cancer Therapy